50% OFF frames with purchase of lenses.
*Restrictions apply. Click here for details.
What is Diabetic Retinopathy?
People with diabetes are at risk for developing diabetic retinopathy: diabetes-related damage to the retina, the light-sensitive tissue at the back of the eye. Over time, high blood sugar harms the retina’s tiny blood vessels, reducing blood flow and causing fluid or blood to leak into the eye, which blurs vision.
In later stages, fragile new vessels can grow and bleed or form scar tissue, increasing the risk of vision loss. Regular dilated eye exams and timely treatment can help protect your sight.
What is Anti-VEGF Treatment?
Anti-VEGF treatment involves injecting a medication into the eye. The medication is placed into the gel layer of the eye, known as the vitreous, and blocks a protein called VEGF, which drives leaky or abnormal blood vessel growth in diabetic eye disease. By blocking VEGF, these medicines reduce swelling in the retina and slow or stop new fragile vessels from forming, which helps protect or improve vision.

How Do Laser Treatments for Diabetic Retinopathy Work?
During laser treatments, your eye doctor will use a calibrated laser to target leaky blood vessels and seal them. This prevents them from leaking further and causing more damage to your retina. If you already have a lot of scar tissue built up from the formation of abnormal blood vessels, the laser can be used to remove it to improve your vision.
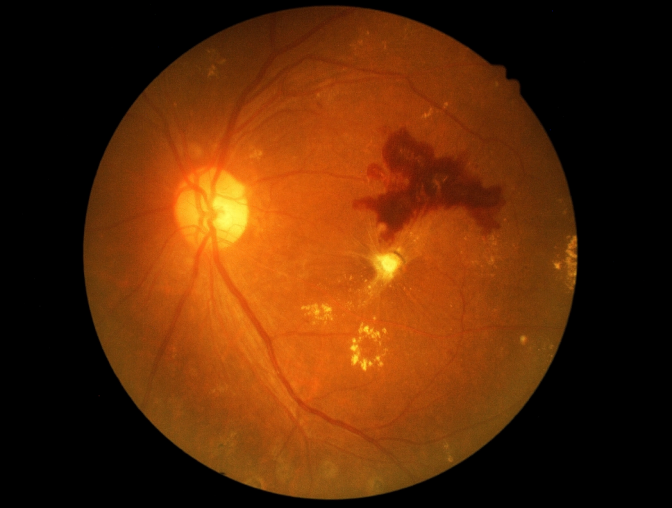
What are the Symptoms of Diabetic Retinopathy?
Diabetic retinopathy symptoms are often silent in the condition’s early stages, and many people may not notice any vision changes at first. When diabetic retinopathy becomes more advanced, it may affect vision in several ways:
Your vision may appear blurry
You may notice floaters in your field of vision
Your night vision may worsen, or you may begin to see colors less vividly
You may see dark spots or unexpected blank areas within your field of vision
If you have diabetes and notice any of these vision problems, call your eye doctor for an appointment to assess your eye health.
Because diabetic retinopathy is an eye disease caused by the symptoms of diabetes, every diabetic should get regularly screened to see if they have it. By the time you finally start noticing symptoms, your vision has already been damaged.
If you have diabetes, schedule regular dilated eye exams after you’re first diagnosed and yearly for type 2, and within five years of diagnosis, then yearly for type 1. Your doctor may recommend more frequent visits if you’re pregnant or have risk factors like poor blood sugar control, high blood pressure, kidney disease, or existing retinopathy.
Schedule an appointment as soon as possible if you notice sudden or worsening blurry vision, new floaters or flashes, a dark curtain over your vision, or eye pain. Early detection and timely treatment help protect your sight.

How Does Clarkson Eyecare Diagnose Diabetic Retinopathy?
Diabetic retinopathy is diagnosed through a comprehensive eye exam, where your eye doctor will assess your retinal health. The doctor will dilate your pupils with eye drops to better examine the inner structures of your eyes and provide an accurate diagnosis.
Other tests include:
Optical Coherence Tomography (OCT): Takes images of the retina to assess its thickness to check for the presence of diabetic retinopathy.
Fluorescein Angiography: Special dye is injected into the bloodstream to highlight damaged and abnormal blood vessels in the eye, which the doctor takes pictures of.
Frequently Asked Questions About Diabetic Retinopathy



Diagnose and Treat Diabetic Retinopathy at Clarkson Eyecare
If you have diabetes and are experiencing symptoms of diabetic retinopathy, don’t hesitate to reach out to our experts. We prioritize comprehensive eye care, ensuring every patient receives the best possible treatment for their vision needs. To effectively manage diabetic retinopathy, find a Clarkson Eyecare location near you and schedule an appointment today.